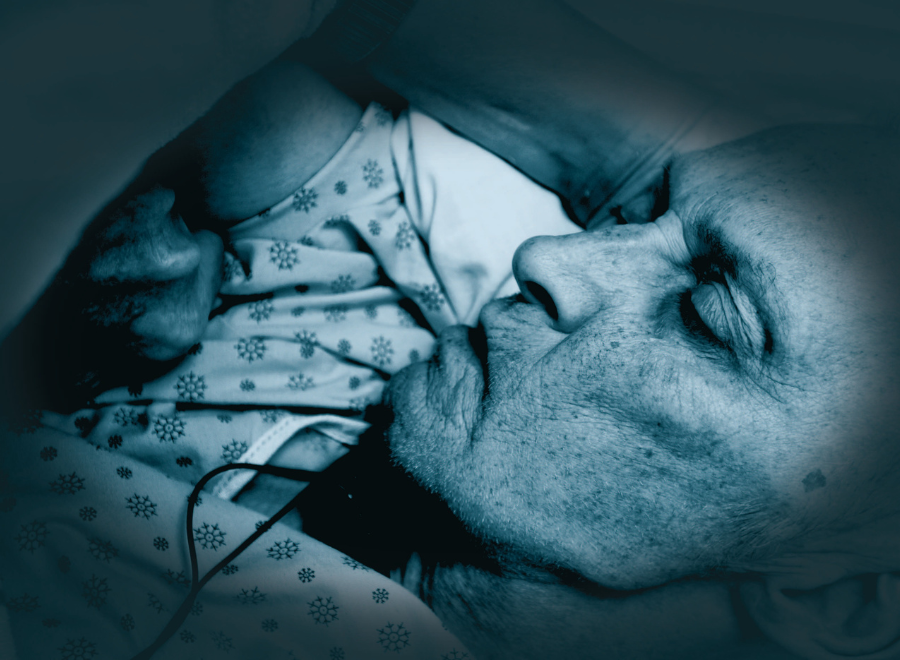
Earlier this year, from his bed in Toronto’s Sunnybrook Hospital, Hassan Rasouli made a thumbs-up sign. It was a simple gesture but it made national headlines.
Since October 2010, the 60-year-old Rasouli has been in a coma, the result of a bacterial infection that followed surgery for a brain tumour. His family has always insisted he is mentally aware but trapped in a paralyzed body. His doctors maintained he was in an irreversible vegetative state and sought court approval to remove him from life support. The thumbs up, which his family believes was deliberate, has since been repeated, adding a new level of complexity to a case that is now headed to the Supreme Court of Canada.
You may unsubscribe from any of our newsletters at any time.
Rasouli’s situation is one of a number of well-publicized events in recent years that have cast end-of-life ethical issues into the national spotlight. From Robert Latimer’s 1994 conviction on charges of murdering his severely disabled 12-year-old daughter Tracy, to Sue Rodriguez’s 1993 legal battle to end her suffering from Lou Gehrig’s disease with the help of a doctor, the issues of euthanasia and assisted suicide are wrenching and divisive.
You’d be correct to think that the roughly 1,000 mostly churchgoing people who completed The Observer’s Life and Death Decisions survey hold strong views on the subject. But you’d be wrong to assume that they are strongly opposed to ending the life of someone who is incurably sick and suffering, or to helping someone end their own life. The most startling finding of the survey is that readers — people of faith who, as a rule, believe life is sacred, a gift from God — are far more inclined to support clinical euthanasia and assisted suicide than members of the general population who completed the same survey.
Elizabeth Murray is one of a number of readers who agreed to be interviewed after the poll results were tabulated. “I have strong views,” says the 79-year-old native of Truro, N.S, a member of Brunswick Street United. “I’m very, very much against keeping people alive for no purpose,” she says. “It’s atrocious.”
Murray practises what she preaches, or perhaps preaches what she has had to practise. “I had a dad who was 92,” she recounts matter-of-factly. “Nothing wrong with him, but he decided his life was over and he stopped eating. Now, I could have kept force-feeding him, but I thought no, that’s just cruel, and he died in a couple of days.” Murray also faced a difficult decision in her mother’s last days. “My mom was 82 when her mind went. Then she got pneumonia and landed in the hospital, and the doctor called me to ask if he should go to extraordinary lengths to keep her alive, and I said no.” Her mother had never expressed a preference, but Murray experienced no qualms, she says: “She was not enjoying life.”
The survey asked respondents to consider six end-of-life scenarios involving euthanasia and two scenarios involving assisted suicide. Respondents were asked whether or not they favoured the measures described in the questions, and how strongly they held their views.
Overall, Observer readers and respondents from the general public declared themselves in favour of euthanasia and assisted suicide. This result was not unexpected. An Angus Reid poll in 2010 found that 67 percent of Canadians support the legalization of active euthanasia, and a Forum Research poll in 2011 found that the same percentage of Canadians favour physician-assisted suicide.
There was, however, a stunning surprise embedded in these results: Observer readers and the general public were miles apart when it came to how strongly in favour of these steps they were. “In all but one scenario,” reported Jane Armstrong Associates, the Toronto research firm that conducted the study, “readers are much more supportive of euthanasia and assisted suicide than are members of the general public.”
The only case where readers and the general population seemed to see almost eye to eye involved a situation in which a family member ends a person’s life when the patient is unable to give consent, and where no prior instruction had been given; this is essentially the Latimer scenario, and it received the least support overall from both groups, with only 29 percent of readers and 25 percent of the general population in favour.
In all the other scenarios, there was a huge gap between readers and the general public. Readers were more than twice as inclined (72 percent to 35 percent) to strongly support a physician and a terminally ill patient agreeing to use pain management medication to hasten death. Eighty-two percent of readers strongly supported a physician and a terminally ill patient agreeing to remove life support, compared to only 48 percent of the general population. And so it goes down the list.
What to make of this? Elizabeth Murray speculates that the response of readers may have something to do with the fact that they are on average older than the population at large. “We see the end of life coming for us,” she says, “and we don’t want to be sitting there with our minds gone and nothing happening.” Murray has made her wishes clear to her five children. “They’re totally in tune with what I feel,” she says. “Do not resuscitate in any way, shape or form. I don’t want to be a burden.”
Canadian law on euthanasia and assisted suicide is complex, according to Bernard Dickens, professor emeritus of health law and policy at the University of Toronto. Some situations are clear-cut, he says. Passive euthanasia — the withdrawal of medical support, nutrition or hydration — is lawful if treatment seems futile to the attending doctor, or if the patient wants treatment to stop.
That’s different from inducing death — active euthanasia, which is illegal. But there are grey areas, Dickens explains. Take “terminal sedation,” for example. Terminally ill patients in pain are usually administered analgesic drugs to ease their suffering. But analgesics can also reduce blood pressure, which doctors know can lead to death. “Everything in this grey area turns on intention,” Dickens says. If the intention is to relieve pain, even in the knowledge that it may bring death a little earlier, that is perfectly lawful medical care, he explains. “If, on the other hand, the intention is to end life, then it is not lawful; it is murder,” he says. “Assisting suicide is also illegal, though here too is a grey area. Failing to provide someone with food on their instruction might be assisted suicide, or not, depending on circumstances.”
Further complicating the legal situation is the inconsistency with which the law is enforced. In January 2010, 89-year-old Kay Carter, a resident of a North Vancouver nursing home who was suffering from chronic spinal stenosis, flew with family members to Zurich, Switzerland, determined to end her own life. (Switzerland, the Netherlands, Belgium, Luxembourg, Colombia and the American states of Washington, Oregon and Montana allow some forms of assisted suicide.) She became the 10th Canadian to commit suicide with help of doctors at a clinic run by the organization Dignitas, but the first Canadian whose death there was openly acknowledged. When it was over, Carter’s daughters mailed letters from Zurich to 120 of their mother’s loved ones. They had not done so beforehand, fearing police intervention. The police never did follow up.
The police did follow up when, in 1997, they charged Halifax respirologist Nancy Morrison with first-degree murder for allegedly dosing throat cancer patient Paul Mills with potassium chloride to hasten his death. A Halifax provincial court judge dismissed the charges on the grounds that there was insufficient evidence to show that the potassium chloride had indeed caused the death of the suffering patient. “She was very rigorously investigated,” says Dickens, “but the whole thing fizzled out when it became clear that she was practising conscientious medicine.”
The growing disconnect between the law and the views of ordinary Canadians, as revealed in the Observer survey and the Angus Reid and Forum research polls, was again evident in interviews with readers. “Sometimes the law is wrong,” says Douglas Allen of Parry Sound, Ont. “It can be based on an understanding of life that is just not appropriate.” Alma Heller of Vernon, B.C., believes euthanasia and assisted suicide should be legalized. But even if not, “If I were terminally ill and in pain and thought there was no hope of improvement, I would rather just finish out my life,” Heller says. Elizabeth Murray, too, wouldn’t let the law deter her from seeking an end to her life if it became necessary. “If I were younger,” she says, “I’d fight the law, but at this point I believe in going ahead with what I think is right.”
While the survey highlights the gap between the views of readers and the general public, it doesn’t explain the reasons for it. In interviews, readers themselves provided some insights. Douglas Allen, for example, grew up in the Anglican Church but recently joined the United Church. The 81-year-old wonders whether the strong support for euthanasia and assisted suicide among readers might reflect the Christian idea that death is a transition, not the end. “With faith we believe that there is something beyond death. You are transformed into another way of being that we know not of, and that transformation needs to be embraced.” Perhaps, he suggests, people of faith are more inclined to view acts that assist the transformation, carried out at the appropriate time in the appropriate way, as benign.
Alma Heller believes that the United Church and its members put a high value on compassion. But this inclination may be amplified by the high proportion of members — and survey respondents — who are women. “Women in the church often are caregivers to older parents,” she observes, “and they’ve been through it. They may have had a parent who is suffering so much they wish they could die, and it makes the caregiver think about it.”
And then there’s the age factor cited at the outset by Elizabeth Murray. The church’s aging membership is often lamented as a challenge for institutional survival, but in the context of the debate over end-of-life issues, perhaps it’s a plus. In addition to Christian compassion, older people bring experience and wisdom to the conversation. One reader, a retired long-term care nurse who asked to remain anonymous, recounted tragic stories from her 20 years in an Ontario hospital to support her firm belief that quality of life must trump quantity.
Retired teacher Charles Letherbridge, 81, of Glencoe, Ont., has lost two wives, his first in 2009, his second in 2011. “Neither of them went through an extended period of illness, but I am certainly thankful they did not,” he says. Many of his friends have not been so lucky. If either of his wives had suffered as he has seen others suffer, “I certainly would have hoped that there would have been some avenue of euthanasia available,” Letherbridge says.
In December, the Supreme Court of Canada will hear the case of Hassan Rasouli, his recent thumbs-up signs notwithstanding. At stake is whether doctors have the right to withdraw life-sustaining treatment they deem to be futile, without the family’s or the patient’s consent. The case is certain to attract intense media attention and spark passionate debate. The Life and Death Decisions survey shows that among the churchgoing readers of this magazine, the debate is already under way — and the direction in which it’s headed is clear. “People have talked to me about this,” says Alma Heller. “They want euthanasia available to them when the time comes, to be available for them to choose if they want it.”
***
This story first appeared in The United Church Observer’s July/August 2012 issue with the title “Choosing a better death.”