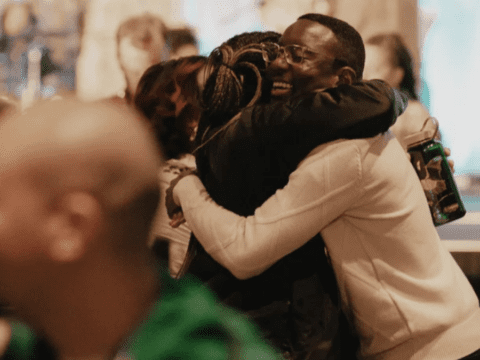I pull two pieces of ID from my wallet, my fingers fumbling, and place a few belongings in the bin before me. After moving through the metal detector, I am directed to walk to the end of a long corridor, where I scrawl my signature in the visitors’ book. The doors click shut behind me. I find a seat and wait, the doubts renewing. Will he wish I hadn’t come?
As soon as we embrace, my fears evaporate. Old feelings of family loyalty and love take over. The next several hours pass quickly as we move into deep terrain — struggles, regrets, worries, longings, plans and hopes — grateful for the chance to reconnect.
You may unsubscribe from any of our newsletters at any time.
I am visiting my nephew, Justin, in the Collins Bay penitentiary in Kingston, Ont. Justin is my age. We grew up together in St. Catharines, Ont., in the 1980s. I remember the two of us dancing as kids to Michael Jackson’s Thriller, riding our bikes around the block and running carefree through the ravine behind my parents’ house. I remember his gifts as an artist — his exquisitely detailed drawings — and his mechanical wizardry as he diligently took apart and resurrected broken radios and television sets.
While he has a way of bringing new life to discarded objects, he has struggled to restore his own life. If you didn’t know him, you might think that Justin, holed up behind these walls for yet another drug-related offence, is just a junkie deserving of our scorn.
As a society, we deny that addicts deserve any dignity or respect. We erect social barriers harder to scale than any prison wall. But if we care to listen, the stories they tell have far more to teach us than the stereotypes that strip them of their humanity.
“I feel like all anyone sees when they look at me is an addict,” Justin says after our hug. “But that’s not who I am.” When I look at him, I see a grown version of the gentle boy I grew up with.
Justin’s mother is my half-sister Rose Mary (surname withheld). But while she and I share the same dad, it is as if we were fathered by different men. The father Rose Mary knew was an alcoholic. By the time she was a teenager, his drinking problem had spiralled out of control. He would often disappear for days at a time, Rose Mary never knowing when, or in what state, he would return.
Rose Mary rebelled with a vengeance. She sought refuge in booze herself, becoming pregnant with Justin at a time when partying, more than parenting, was her priority. Justin’s father wasn’t in the picture for long, and the stepfather who replaced him abused both mother and child. Rose Mary remembers her small son waiting expectantly for his biological father to visit, only to be crestfallen when he didn’t arrive; his stepfather then made sure that Justin’s sadness turned to fear.
I was conceived when my father was 40. By then, his harrowing journey with alcohol — the aftermath of his own painful past — had come to an end. Justin’s battles were just beginning.
He was still a little kid when he started stealing; he has no idea why. “Adrenalin, maybe,” he speculates. “I always felt stressed.” Next came the drugs and alcohol. Around the time I was leaving home for university, Justin was going to a juvenile detention centre to serve his first sentence on a drunk driving charge. Then came rehab, but instead of recovering, Justin descended deeper into depression. After coming home, he couldn’t get out of bed.
“What’s depression?” he asks me. “It’s just a word. Most people have no idea what it feels like. You can’t eat. You can’t sleep. You are in such spiritual darkness. It’s torture. You’ll do anything to make it end.” Telling someone who is depressed not to reach for drugs is like telling someone who is thirsty not to drink a glass of water, he tells me. If there’s something that will lessen the agony, even temporarily, you’re going to take it.
Justin’s experimentation with harder drugs — crack cocaine, heroin and a cocktail of pharmaceuticals — coincided with a litany of medical diagnoses. He has been told he has borderline personality disorder and ADHD. In this, Justin is like many survivors of childhood trauma: it’s hard to know where the mental illness ends and the addiction begins.
A growing body of research suggests that both genetics and outside circumstances contribute to addiction. The physiology of the brain is rewired, neuroscientists believe, through early traumas like abuse and abandonment, leading to an increased susceptibility to addiction.
Perhaps the most far-reaching research is the Adverse Childhood Experiences (ACEs) study, conducted by California-based Kaiser Permanente and the U.S. Centers for Disease Control and Prevention. In the late 1990s, the study examined the significance of early painful experiences across 10 categories — including domestic violence; physical or sexual abuse; and drug abuse, incarceration or mental illness in the family. The data showed that subjects with five or more ACEs had a seven to 10 times higher prevalence of substance abuse compared to those with no ACEs.
Other research suggests that drugs, in and of themselves, do not necessarily lead to addiction. What does, according to Dr. Gabor Maté, a renowned physician and author who worked in Vancouver’s Downtown Eastside, are “emotional isolation, powerlessness, and stress.” These, he writes in his 2008 book, In the Realm of Hungry Ghosts: Close Encounters with Addiction, “are exactly the conditions that promote the neurobiology of addiction.”
In the 1970s, psychologist Bruce Alexander of Simon Fraser University in Burnaby, B.C., built a large enclosure for lab rats that he called the Rat Park. Full of stimulating activities and social opportunities, it was the opposite of the solitary, uninspiring environment usually experienced by rats in addiction studies. With little to do other than imbibe the drugs that were left for them, rats in the typical lab setting easily became hooked. In “Rat Heaven,” as Alexander’s enclosure is sometimes called, rats almost always preferred water to morphine; they rarely used drugs, and they never overdosed.
A study of soldiers returning from Vietnam during the 1970s suggests that humans respond similarly. While as many as 20 percent of soldiers became addicted to heroin overseas, 95 percent of the addicts simply stopped using the drug when they left the confines of military life.
The Rat Park experiment, while not without controversy, supports a seismic shift in how some researchers now understand addiction. What addicts are searching for in substances, many would agree, is simply a substitute for human trust and security. To borrow the words of British journalist Johann Hari in his popular TED Talk on the subject, “The opposite of addiction is not sobriety; the opposite of addiction is connection.”
I ask Justin what he thinks about this theory, and he says it’s bang on. He tells me that addicts are looking for brief moments of connection that only drugs seem able to provide. He says he’s had some of his deepest philosophical conversations and most meaningful emotional connections in crack houses.
We talk about how incarceration isolates people who already feel alienated, making it harder for them to adjust to the outside world and more likely to reoffend. “No wonder the prison industry is booming,” Justin remarks.
Then I ask him a question that troubles me and others. Does any of this justify committing a violent crime? Justin is in jail because he held up a store clerk at knifepoint three years ago. He says it was an act of desperation committed in the darkest hour of depression. His friends and family, all disillusioned by his increasingly erratic and impulsive behaviour, had distanced themselves. He was at rock bottom with no one to turn to and no positive options. As he explains, when there’s no way for change to happen for the better, you’ll take the bad. “I wanted to get caught,” he says. “I knew I had to do something. I knew prison would at least be a change.”
Some might worry that Justin’s narrative of abandonment is a way of avoiding accountability. But others wonder if a little compassion could encourage offenders like Justin to begin to hold themselves accountable for their crimes. “I’ve always been fond of the Jewish adage that you should not punish someone so harshly that they forget what they’ve done,” says former Correctional Service Canada chaplain Kate Johnson of Kingston, Ont. “When prisoners face unnecessarily punitive conditions, their survival instincts often overwhelm their capacity for reflection. Victims’ needs for accountability and amends-making will be more easily met when we have responses to crime that allow offenders to be educated, to empathize and in turn to hold themselves accountable.”
Clearly, the hardline approach isn’t working. Drug addiction in Canada is escalating; so is the number of addicts winding up in prison. Correctional Service Canada says up to 80 percent of offenders entering the federal prison system these days have some sort of substance abuse problem.
Might the answer be fewer prison sentences? There’s reason to believe that decriminalizing drugs, coupled with innovative social programs, could provide a better way. Portugal offers a promising prototype. In 2001, the country took the radical step of decriminalizing all drugs, treating possession of small quantities of everything from marijuana to heroin as an issue for public health, not for the criminal justice system. Money once spent on imprisonment was channelled into counselling services, subsidized jobs and rehabilitation. “The goal,” Johann Hari says in his TED Talk, “was to make sure that every addict in Portugal had something to get out of bed for in the morning.” The approach has reduced the country’s addiction rates and cut the number of people in prison for drug offences in half.
Most addicted prisoners in Canada will experience more of the same fear and violence in prison that led to their incarceration in the first place, and will likely return to petty crime and poverty upon release. As Maté writes, any good that prison might do is outweighed by the bad: “While on the positive side, jail at times gives people a much-needed break from their compulsive drug use, on release most will relapse into drug taking and, of necessity, into the illegal acts required to sustain those habits.”
He could have been talking about Justin.
After serving a third of his three-year sentence for the 2014 armed robbery, Justin was eligible for parole in the fall of 2015. My father, now in his 80s and sober for decades, agreed to be his parole guarantor. The conditions were straightforward: no alcohol and no drugs.
Reality, however, was far more complex. My parents found themselves woefully unprepared for the road ahead. “We had no idea what we were walking into,” my mother says, noting that they had almost no support and no real awareness of the severity of Justin’s problems.
Justin arrived in Elliot Lake, Ont., with big dreams and daunting challenges: debts to pay, the stigma of a criminal record, the curse of persistent cravings and the chronic pull of depression. Even so, his prospects seemed better than ever.
After the isolation of jail, Justin rekindled his family relationships. He became a frequent fixture in my brother’s home, basking in the attention of his younger cousins — small children who didn’t judge or fear him but loved him unreservedly. He also took to working on occasion in the family business. He had always been gifted with his hands, and now he was busy building and fixing things. We all held our breath and hoped for the best.
Just before Christmas in 2015, crisis struck. Justin had an accident while using a saw and lost three fingers. We all knew what this meant: prescription painkillers. To help him cope with the extreme pain, Justin was prescribed Percocet — one of the opioids he was addicted to. We waited, and we worried. My father struggled with mounting anxiety and insomnia.
Slowly, we noticed small signs of overuse: Justin slept a lot; his personal appearance deteriorated; he withdrew. He was desperate for Percocet refills. His behaviour gave us reason to suspect he might also be using street drugs again.
One day when my father was outside his own apartment building, he heard loud moaning. When he entered the apartment, he found Justin unconscious and called the paramedics. Then, because the overdose meant Justin had broken his parole conditions, my father called Justin’s parole officer.
The next week, my parents watched as their grandson was handcuffed, placed in a police car and driven back to Kingston. We were all heartbroken, especially my sister, who has endured the cycle of guilt, self-blame, desperation and hope for more than 20 years now.
Easter will mark the end of Justin’s sentence. He will be 40 when he is released. Redemption feels elusive. Our hopes are mixed with the familiar dread that we are about to resume our parts in a tragic play whose predictable plot we cannot alter.
My visits with Justin did nothing to abate my fears. He is consumed with anxiety about life on the outside. He doesn’t know where he will go, how he will make ends meet or what he will do with his life. He tells me he is considering surgery to have the final finger on his left hand removed; the one digit is awkward. Stress, surgery, prescription painkillers: I think I know how that story ends.
Still, I hold out hope that the ending to this new chapter will be a surprise. I know Justin well enough to appreciate that for all his mistakes and wrong turns, he is an exemplary human being. He values people and listens to their stories, regardless of their status or situation.
But as my father is fond of reminding me, every addict is a Dr. Jekyll and Mr. Hyde: the sane, loving person can suddenly give way to a selfish, angry and irrational manipulator. And when addicts go down the rabbit hole, they take their loved ones with them.
My sister has said the only peace she knows is when her son is in prison. When Justin is out, she is perpetually on edge with worry, always on the brink of a breakdown. She would be the first to tell you that loving an addict is debilitating: addiction terrorizes and traumatizes loved ones over and over again. In Rose Mary’s case, she has suffered paroxysms of rage and despair that mere prose could never fully describe.
As we await Justin’s release, we struggle to know how to support him in a way that is healthy and healing. Justin already feels let down by us. His recent requests for financial help have been turned down by family whose fear and mistrust are well founded. From Justin’s perspective, he needs us to reach out in faith if he is to find his way forward and make a fresh start. I wish I had the answers. For now, all I can do is sit with him in this space, listen to him as another human being with thoughts and feelings as valid as my own, and love him for who he is. I don’t know if that will be enough. Justin has grown fond of the prison routine, of his small cell and of the people he has met: he has discovered a sense of community inside these walls that has eluded him all his life. “There is a level of love and solidarity in here that you would never find on the outside,” he says, “not even among family.” And then he adds, with a touch of premature nostalgia, “I will miss it here.”
This story first appeared in The Observer’s April 2017 issue with the title “The trouble with Justin.”