Photography by Tallulah
On a warm March day last year in Kenya’s bustling capital city of Nairobi, about 20 patients gather in the shady outdoor reception area of Platinum Surgery Center. But rather than quietly talk about spouses or lovers, children or jobs, the conversation focuses on one thing: FGM/C — female genital mutilation or cutting. “We shared the terrible stories and what every person went through — this thing that we were hiding for many years,” says Christine,* a 31-year-old Nairobi businesswoman with neon-pink fingernails and a bright smile. “You pour your heart out to these ladies.”
You may unsubscribe from any of our newsletters at any time.
The women, not only Kenyan but also Somali, Sudanese and Tanzanian, aged 21 to 65, all underwent FGM/C as girls or teens. After years of dealing with the physical and psychological effects of this practice — which predates both Islam and Christianity and is said to have been started by the pharaohs of ancient Egypt — they are here to try to become whole again. For some, this means urinating and menstruating normally. For others, it means orgasming for the first time.
The waiting area at Platinum, owned by Kenyan plastic surgeon Dr. Abdullahi Adan, is filled with trepidation as well as anticipation. Not all of these women will be candidates for clitoral reconstructive surgery. Like 200 million girls and women around the world, they had part or all of their external genitalia sliced off — usually without anesthetic — by women called “cutters,” using implements such as unsterilized razor blades, scissors or broken glass. Another 3.9 million girls are at risk of being cut every year.
Many see FGM/C as the ultimate expression of the subjugation and control of women by society. But an awakening is underway, with women in places where FGM/C is commonplace raising their voices in protest. Adding to the groundswell are the actions of the medical community, interest groups, and NGOs like Clitoraid, an American humanitarian agency that helps fund this restorative surgery in Nairobi. Such groups are bolstering a grassroots movement that includes specialized care for survivors, as well as preventive initiatives to upend this tradition.
In the waiting room, Christine fervently prays to God: “Let me be one of the people who will be going through the surgery.” The memory of being held down at age nine, having her clitoris sliced with a razor blade, still haunts her and affects her self-esteem. With modern, urbanized Kenyan men increasingly rejecting FGM/C, encountering a cut woman is becoming less common. Christine recalls the shame she has felt when shocked lovers exclaimed, “Where is your clitoris?” She says, “It made me feel bad — less of a woman.
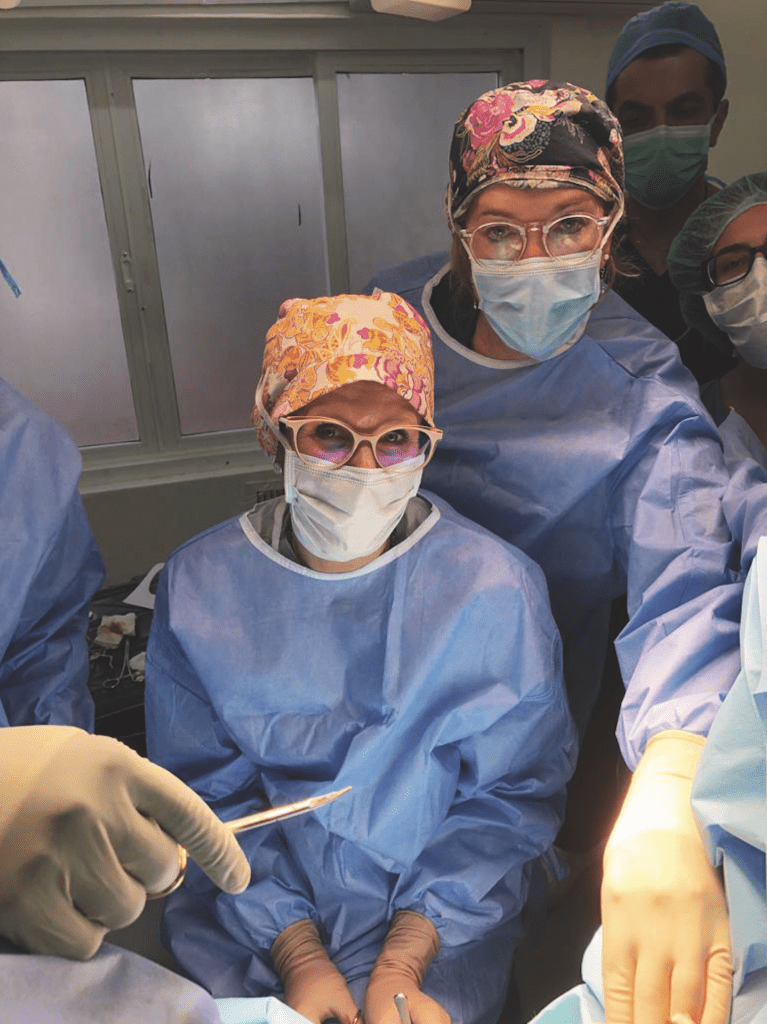
Eventually, Christine is examined by Dr. Angela Deane of Calgary, one of three visiting surgeons from Canada, the United States and Australia who have arrived in Kenya for a 10-day volunteer mission to help FGM/C survivors. Deane, who has long blond hair and quirky pink glasses, is gentle and patient, upholding the gynecological principle of consent, knowing that FGM/C survivors can suffer anxiety and post-traumatic stress disorder. “May I examine you? Is there pain? Where?” And, “Do you want to look with me?” If yes, Deane gives the patient a mirror. This by itself can be traumatizing, as many women have never viewed themselves this way.
Deane approves Christine for surgery, which is undertaken by Dr. Marci Bowers of California, a world-renowned physician who specializes in transgender surgery. Bowers took Deane under her wing shortly after the pair met late in 2018 in Calgary. Bowers has treated many patients from Canada, and always wanted a Canadian colleague to help relieve the demand. Deane was the perfect protege.
More on Broadview: I underwent FGM. It doesn’t define me
Upon her return to Calgary after the mission last March, Deane began researching the medical community’s training on caring for FGM/C survivors, including reconstructive work and delivering their babies. Deane is an OB/GYN resident at the University of Calgary, and she launched a study, surveying family physicians, OB/GYNs, plastic surgeons, obstetrical nurses and midwives, probing their understanding and attitudes toward FGM/C and the scope of care they were able to provide.
Deane’s preliminary findings indicate that the greatest barrier to proper care is a lack of training, with only nine percent of respondents stating that they felt very prepared to provide adequate treatment to FGM/C survivors. Knowledge gaps include the short- and long-term complications associated with FGM/C or even how to obtain a proper medical history of survivors. “Canada is far behind the rest of the world in how we treat women who’ve been cut,” says Deane. “There are so many layers of complexity and culture that Canadian physicians don’t have the skills to address. We also lack training for nurses and midwives.”
The World Health Organization classifies FGM/C into four different types. Type 4 is the least invasive and can involve genital pricking and/or piercing. Type 3 is the most severe and at its worst involves a clitoridectomy (removal of part or all of the clitoris), as well as removal of the inner and outer labia. The wound is then infibulated, or stitched together, drastically narrowing the vaginal opening. Depending on the type of FGM/C, the practice can hinder urination and menstruation, leading to odour, infection, cysts and shame. It can make sex excruciating and cause childbirth to be dangerous for both mother and baby.
A woman who has undergone FGM/C is especially vulnerable to prolonged labour, vaginal tearing and excessive bleeding. For some, if their scarred, narrow genitalia isn’t first deinfibulated — a surgical procedure to widen the vaginal opening — their babies are at higher risk of complications and even death, as they cannot be pushed out the birth canal. Sometimes a caesarean section is needed to ensure safe delivery.
Interestingly, the very anatomy of the clitoris is what makes restorative surgery possible. Starting from the glans (the external part of the clitoris), the clitoral tissue extends two to four centimetres before splitting in half and running another five to nine centimetres under the muscle alongside the vagina toward the anus. The surgeon can bring forth a portion of this tissue and rebuild it into an external clitoris. With therapy following surgery, sexual pleasure is achievable for many.
Other countries far exceed Canada in offering help to FGM/C survivors. In the United Kingdom, for example, the recently opened National FGM Support Clinics provide a full range of multidisciplinary health services and counselling. And in France, surgeon and urologist Dr. Pierre Foldès, who pioneered the clitoral reconstruction technique around 2004, still performs corrective surgeries and trains other physicians to do the same.
Here in Canada, at least 80,000 women have suffered FGM/C — the vast majority immigrants from other countries, according to the End FGM Canada Network. As an OB/GYN resident, Deane assists women who arrive in labour at Calgary’s hospitals, including at the Peter Lougheed Centre. She estimates that one to four per month are FGM/C survivors. The hospital is in the city’s northeast, home to many immigrants and refugees from African countries such as Sudan, Djibouti, Somalia, Eritrea and Egypt.
Deane is developing an information session on FGM/C that will be incorporated into the curriculum at Cumming School of Medicine where she studies. She hopes it will encourage other medical schools to expand their curricula and embrace enhanced medical care for FGM/C survivors.

FGM/C is said to mark the passage from girlhood to womanhood. In reality, it is an expression of patriarchal control. In most cases, the primary intent of the practice — which can make sexual intercourse painful, uncomfortable or devoid of sensation — is for a girl or woman to keep her virginity until marriage and, once married, not be tempted to have sex outside the conjugal bed.
FGM/C is considered a violation of human rights by the World Health Organization and UNICEF. Deane recalls one Kenyan woman at the Clitoraid clinic describing the day she was cut as the moment “her inner light went dim.” “It is gender inequality, 100 percent,” Deane says. “And until women can decide for themselves about their own body, this will persist.”
While therapy and reconstructive surgery can help survivors, more work needs to be done to prevent FGM/C. Sweden displays ads on buses with a helpline for girls at risk, and some European countries recommend that girls who suspect they are being sent abroad to undergo FGM/C put a spoon in their underwear. This sets off an alarm at airport security, and staff take the girls aside to discuss their fears and concerns.
In the United Kingdom, the National Society for the Prevention of Cruelty to Children (NSPCC) set up a dedicated helpline in 2013 to assist those at risk of FGM/C. Between the summers of 2013 and 2019, the NSPCC fielded over 2,700 calls — nearly one in five of them “so serious they were referred to external agencies,” the NSPCC reports. Starting this year, secondary schools in England are required to teach about FGM/C.
In Canada, the Criminal Code was amended in 1997, declaring FGM/C aggravated assault, punishable by up to 14 years behind bars. It is also illegal to take a girl to another country to carry out the act, although some families continue to send their daughters to regions in the Middle East or to African countries such as Somalia, Egypt, Sierra Leone, Mali, Sudan and Eritrea, places where UNICEF reports cutting rates are as high as 98 percent.
The End FGM Canada Network is pushing Ottawa to create a national action plan to support survivors and protect girls at risk of FGM/C. Canada, says the organization’s co-founder Giselle Portenier, needs to follow the lead of other countries and set up helplines and airport protections to assist girls who fear they will be cut. As it stands, Canada has no such measures in place. “We’ve sacrificed the human rights of children,” says Portenier, also a filmmaker, whose 2018 award-winning documentary, In the Name of Your Daughter, discussed FGM/C in Tanzania.
While Canada tries to respond to this issue more effectively, some of the most important advocacy work is being done by women, many of them survivors, in the countries where FGM/C is most commonly practised.

A line of teenage Maasai girls stomp their sandal-clad feet in percussive unison, raising puffs of tawny dust while chanting a high-pitched song. Their dance is part of the noisy and jubilant closing ceremony of the three-day, community-led Alternative Rite of Passage (ARP). It was held last August at Iltilal Primary School in Kajiado, a region of southern Kenya where up to 95 percent of girls in the Maasai community are being cut.
For the Maasai teens, wearing white silken purity scarves and colourful, ornate necklaces, chokers and bracelets with beaded geometric designs, the event signals a profound cultural shift. Unlike many of their older sisters, mothers and grandmothers, these girls have not undergone FGM/C. And they have embraced the change, wearing bold broad ribbons around their foreheads stating “No F.G.M.”
Amref Health Africa, a non-profit organization, first developed ARPs in collaboration with local communities in 2009 as an alternative to FGM/C ceremonies, which mark girls’ transition to womanhood. The three-day celebration provides young Maasai with sex education as well as self-esteem building exercises to help empower girls to say no to cutting. Participants are given emergency numbers to call if they fear there are plans to have them cut.
To boost its acceptance among older generations, the ARP ceremony includes community elders and women who used to be cutters, and mimics in duration the original rite of passage that previously accompanied the cutting of girls. Jane Nkoitai, 15, is one of 545 female and 88 male young people participating in the event. Speaking through a translator, Nkoitai says that she is “very happy I’m not going through the cut. I want to continue my education and become a doctor and change the community.”
Abdi Mohamed, 19, spoke at the ceremony, boldly exclaiming to the crowd of more than 1,000 people, “If you cut your girl, I will not marry her!” sparking laughter and a rousing cheer from the crowd. Afterwards, Mohamed states that the best way to end FGM/C is through education: “We hope one day it will be history.”
Many people, especially survivors like Christine, also hope that FGM/C will one day be relegated to the history books. Right after her clitoral restoration at the Platinum Surgery Center, Christine says she felt an immediate difference — a release. She laughs as she admits launching into a hymn called I Thank You God from her surgical bed.
Now, she doesn’t fear marriage or dread lovers’ scorn. “I’m new,” she says. “My life is changed.”
This story first appeared in Broadview’s March 2020 issue with the title “Healing all wounds.”
Broadview is an award-winning progressive Christian magazine, featuring stories about spirituality, justice and ethical living. For more of our content, subscribe to the magazine today.














This is a crime and it should not ever happen to anyone. We are interested in the reconstruction surgery
Hopefully FGM will be ended soon. It is barbaric. However, while we’re at it, let’s end the other barbaric act of sexual abuse as well: circumcision. There’s no need for it except in some medical cases. It is an ancient religious practice born out of misguided faith and superstition.
Hello, I’m Frances F. Pency from Liberia.
I’m a victim and survivor of FGM since 1985 at age 10, and with complication in childbirth.
Born on August 19, 1975.
I just read the story of this survivor who got reconstruction surgery, and she is proud of herself today. I’m happy for her and I wish to be like her. Please help me get this surgery , I’m begging you all in the name of our Lord and Savior Jesus Christ.
I’m a Liberian, writing you from Monrovia, Liberia. God bless you all,
Kindest Regards
Frances F. Pency